
Part D Cost for Brand Name Drugs Rising
Reforms to Medicare Part D under the Affordable Care Act brought significant relief to retirees by reducing the share of medication costs they must pay out of their own pockets.
But with the healthcare reform now nearly a decade old, other developments have taken over that will drive up drug costs for the most vulnerable retirees – the biggest users of expensive brand name drugs. Although only a few million people will be affected, they are already saddled with the highest spending burden.
This vulnerable group could get some help from Congress. There is bipartisan support for placing an absolute limit on how much Part D policyholders must pay in total for their prescriptions, said Juliette Cubanski, associate director of the Medicare policy program at the Kaiser Family Foundation.
“That’s a positive development,” she said, “but there are also several areas of disagreement in the legislation being considered on the House and Senate sides.”
Under the Affordable Care Act (ACA), retirees are required to pay 25 percent of their total drug costs up to the annual threshold that qualifies them for catastrophic coverage – this dollar threshold is the total of their own payments plus the price discounts from manufacturers of brand name drugs. The upshot in 2020 for retirees is that those with the highest need could spend about $375 more out of their own pockets before they enter Part D’s less-onerous catastrophic coverage phase, according to a Kaiser analysis. And that’s just the increase for next year – their outlays will rise over the next decade. 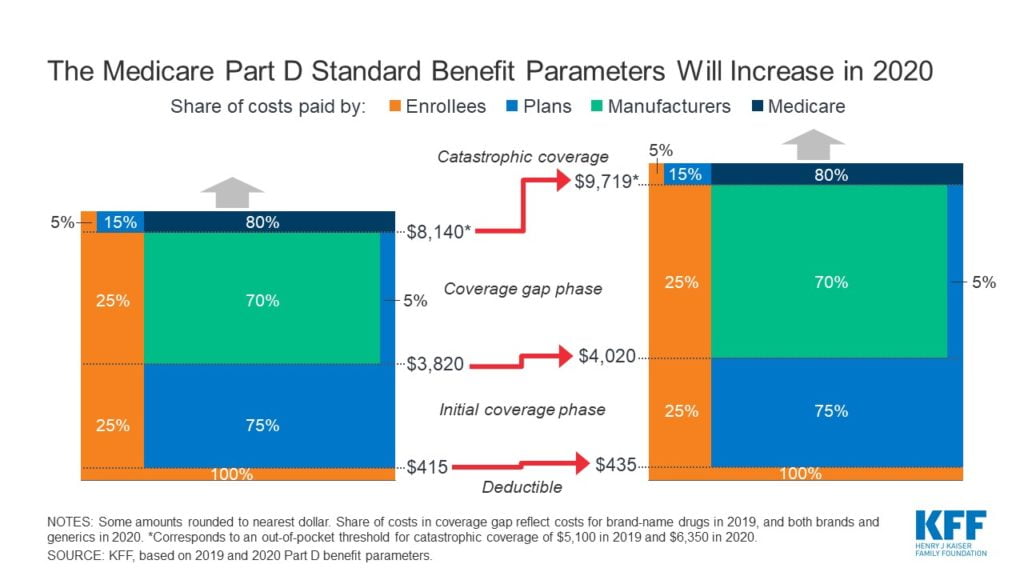
Once retirees enter the catastrophic phase, they are protected, because Medicare begins picking up the vast majority of the tab. But out-of-pocket costs are rising because the ACA’s controls on the spending threshold they must cross to qualify for catastrophic coverage have ended.
In 2020, this threshold – their own spending plus the subsidies – will rise to $6,350, up from $5,100 in this year. Over the next decade, the threshold will nearly double. Previous years’ increases were about $150. As the threshold increases, the dollar amount retirees will pay directly out of their own pockets will rise with it. On top of that, retirees’ deductibles and required payments in the initial cost-sharing phase of coverage (see chart), will increase every year too.
Under Part D’s catastrophic coverage, retirees pay only 5 percent of a drug’s total cost. But a second, fairly recent, development is eroding this protection too: escalating prices for expensive brand name and specialty drugs. Annual purchases for arthritis, hepatitis C, and leukemia medications, for example, can add up to $10,000 or more per year and take a substantial bite out of retirement income.
People who take only generic drugs could also see increases in their out-of-pocket spending, because the prices for generics are not subsidized by manufacturers. In reality, though, most generics cost less than brand name drugs, and retirees who rely on them typically spend much less on their medications overall.
While their drug spending is accelerating, Cubanski said the complex way that out-of-pocket outlays are calculated makes it virtually impossible for retirees to anticipate how much they will spend in the coming year.
Squared Away writer Kim Blanton invites you to follow us on Twitter @SquaredAwayBC. To stay current on our blog, please join our free email list. You’ll receive just one email each week – with links to the two new posts for that week – when you sign up here. This blog is supported by the Center for Retirement Research at Boston College.
Comments are closed.







Drugs costs in the U.S. are vastly higher than in most countries for the simple reason that we have allowed the pharmaceutical companies to get away with it. Drug costs have risen much faster than overall medical costs, which in turn have risen much more than the general cost of living. We are now faced with ‘designer drugs” with price tags in the $ millions. It is time to goad Congress into ignoring the money Big Pharma spends on lobbying and allow Medicare to negotiate drug prices as the VA and DoD do. Read my book and get angry! Prescription for Bankruptcy.
Drugs costs in the U.S. are vastly higher than in most countries for the simple reason that we have allowed the pharmaceutical companies to get away with it. Drug costs have risen much faster than overall medical costs, which in turn have risen much more than the general cost of living. We are now faced with ‘designer drugs” with price tags in the $ millions. It is time to goad Congress into ignoring the money Big Pharma spends on lobbying and allow Medicare to negotiate drug prices as the VA and DoD do. Read my book and get angry! Prescription for Bankruptcy.
Dr. Hoffer – thanks for including the “And How We Can Fix It” phrase to the title of your book. I’m so angry about so much in the public sector now — especially our health care system — I’m not sure I can take any more! I’ll put the book on my xmas list, although I don’t think I need any more data to know that big pharma is scamming Americans big time … and our duly elected representatives are enabling them. Here’s what one Senator, John Thune, said about proposed legislation to allow Medicare to negotiate drug prices: “It’s a huge government intervention in the drug marketplace, with a lot of price-setting. And the government [is] basically taking over a private industry. It’s really bad policy and I think it’s dead on arrival over here.” When big business uses market clout to fix high prices, it’s the free enterprise system. When government uses market size to negotiate lower prices, it’s price-setting and socialism. Disgusting.
So here is the situation with the present Medicare Part D situation in the United States: why would Congress past a LAW that prohibits Health and Human Services from negotiating drug prices for Medicare Part D when they are owned by the health care lobby? The Veterans Administration buys the same drugs at a 70% discount to Part D. Second, the catastrophic threshold is going up almost 25% a year with an inflation rate of 2.5%, and these drugs already have the Research and Development cost built in them, so it is all about profits. When are citizens going to demand action and where is the AARP?